At the Steve Gleason Institute, adaptive technology improves ALS patients’ lives
Theresa Whitlock-Wild’s husband, Matt, was diagnosed with ALS in his early 40s. Shortly afterward, the couple had their home remodeled, and they would have benefited from some expert advice.
Standard ADA design didn’t fully accommodate the 600-pound wheelchair Matt Wild—a six-foot, three-inch former US Marine—would eventually use. Nor was the couple familiar with how adaptive technology could improve his quality of life as the disease progressed.

(Multi-exposure photo Cori Kogan)
“When you get this diagnosis, you have to make a lot of decisions quickly,” Whitlock-Wild says. “I wish someone would have held my hand and said, ‘OK, now we need to think about this.’”
Whitlock-Wild is the project manager for the Adaptive Technology Center (ATC) at Washington State University Spokane. Part of the Steve Gleason Institute for Neuroscience, the center showcases devices that simplify daily tasks for caregivers and people with ALS (amyotrophic lateral sclerosis), a disease that leads to eventual paralysis.
At the center, ALS patients can turn on kitchen faucets and open microwaves with voice-activated smart home features. They can use computers or play video games with chin or breath controls. And they can learn how eye-gaze machines and voice banking will help them communicate after they lose the ability to talk.
Many of the devices aren’t covered by insurance. A bed on display allows patients to reposition themselves with eye-gaze or voice commands. The cost: $45,000.
Trying out adaptive technology helps people prioritize where to put their resources, Whitlock-Wild says. “We help inform, so patients and families can make the best decisions for themselves.”
The center is the public face of the Gleason Institute. Established in 2019, the institute is named for Spokane native Steve Gleason (’00 Busi.), a Cougar linebacker and NFL player for the New Orleans Saints. After his 2011 diagnosis, Gleason became an advocate for ALS patients, receiving a Congressional Gold Medal for his work.
Besides helping families, the institute brings together research at WSU and community partners such as the Providence Neuroscience Institute and St. Luke’s Rehabilitation Medical Center. Ken Isaacs, the Gleason Institute’s director, is a neurologist who holds a joint appointment with Providence.
The initial $500,000 in funding came from the Health Sciences and Services Authority of Spokane County and an Avista subsidiary. Gleason’s nonprofit, Team Gleason, and other companies donated adaptive equipment.
“Steve Gleason has embraced adaptive technology in his daily life,” says Andrea Lazarus, associate vice president for WSU Health Sciences and the institute’s executive director. “But the value of these technologies is not limited to ALS—they’re for anyone with mobility limitations.”
With an initial focus on ALS, the institute will eventually expand to other neurodegenerative diseases, such as Parkinson’s, multiple sclerosis, and Alzheimer’s. Besides adaptive technology, the institute researches new therapies, disease risk factors, and stress reduction for caregivers.
“There are pockets of neuroscience research throughout the university—from drug discovery in the College of Pharmacy to English department faculty who want to study how journaling affects caretakers’ well-being,” Lazarus says. “We’re also a catalyst for connecting researchers and health professionals for clinical trials.”
More than 150 years after ALS was identified by a French neurologist, many aspects of the disease remain a mystery. Scientists aren’t clear what causes the motor neurons to degenerate and stop sending messages to muscles. In a small number of patients, heredity is a factor, and chemical exposure also appears to heighten the risk. Military veterans are about twice as likely as the general public to develop ALS.
Each year, about 5,000 US residents are diagnosed with ALS. Most patients die within two to five years, although some live much longer.
Besides patients and families, Whitlock-Wild gives tours of the Adaptive Technology Center to students ranging from junior high to medical school. Her husband was diagnosed with ALS about eight years ago. She wants to expose students to some of the challenges of living with a debilitating disease and the toll it takes on families.
Using an eye-gaze device requires hours of practice. “Some of these students are in occupational therapy and haven’t had a chance to try out this type of equipment,” Whitlock-Wild says. “They should know how difficult it is.”
“The Adaptive Technology Center has done a lot for patients and families,” says Linda Sprenger, whose late husband Mike had ALS.
When the couple visited the center in 2021, Mike couldn’t keep his eyes open long enough to use his eye-gaze device. But he could still twitch an eyebrow. “We spelled things out to ask if he was hot, if he was cold, if he wanted to change the channel,” Sprenger says.
At the center, Mike tried out another machine that utilized his remaining muscle movement. “Suddenly, there were words on the screen,” Sprenger says. The different technology extended the time Mike could communicate with family and caregivers.
A future phase of the center will include space for testing prototypes of new devices.
“We look at the Adaptive Technology Center as welcoming not only for patients and their families but for entrepreneurs and others who can help improve their lives,” Isaacs says.
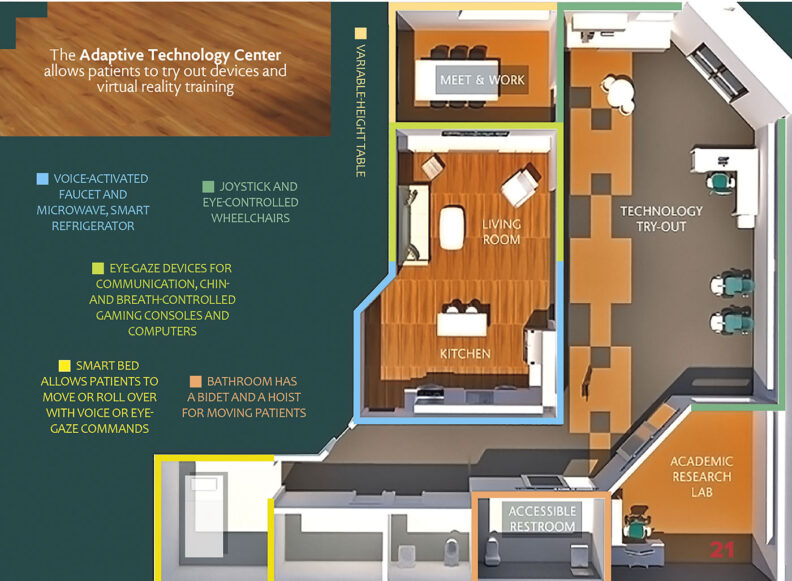
Click on image for full-screen infographic (PDF)
Read more
Adaptive Technology Center at the Steve Gleason Institute for Neuroscience
Gleason Institute helps users experience the joy of adaptive gaming (WSU Insider, Oct. 11, 2023)
No white flags (Spring 2016, Washington State Magazine)
Steve Gleason named Regents Distinguished Alumnus (Winter 2017, Washington State Magazine)
