Spokane hospital executives grew increasingly anxious as they scoured the ominous headlines late last winter. COVID-19 cases were multiplying rapidly in the Seattle area, and eastern Washington agencies felt ill-equipped to handle a similar surge.
In an effort to prepare, the CEO from the Inland Northwest Region of the MultiCare Health System, which runs Deaconess Hospital and Valley Hospital, reached out to John Tomkowiak, the founding dean of the Elson S. Floyd College of Medicine at Washington State University Health Sciences Spokane.
Their request was for a web-based modeling tool that could help predict hospital needs such as gowns, gloves, N95 masks, and ventilator beds. MultiCare envisioned such a tool would be simple to operate and accessible anywhere in the world.
The idea landed on the desk of Ofer Amram, assistant professor in the Elson S. Floyd College of Medicine and director of the Community Health and Spatial Epidemiology (CHaSE) Lab. Amram and his colleagues use statistical modeling to study the relationship between space, place, and public health outcomes.
Amram shared the proposal with Sterling McPherson (’08 MS, ’10 PhD Psych.), associate professor and assistant dean for research in the college of medicine.
“Sterling and I started developing the hospital capacity tool around mid-March when west side cases were ramping up on a daily basis and it was starting to get bad in New York,” Amram says. “At that point, there were a lot of predictions saying there would be over 50,000 deaths. It seemed like a big storm was coming and MultiCare wanted to plan for the worst.
“For two or three weeks, we worked with MultiCare on a daily basis as it was a period of great urgency and uncertainty about what was going to happen,” he says. “We were studying the doubling rate of COVID cases in the community, and then, based on the projection of incoming patients, trying to determine what that meant in terms of equipment and personnel.
“It was really intense. We were asked to create reports every day for MultiCare, the Spokane Regional Health District, hard-hit Yakima hospitals, and other areas. For the first few days, it looked really bad for our region, but the model helped us get a grip on managing supplies.”
At the time, Amram says Spokane city leaders were preparing community centers to hold overflow COVID patients if necessary, but fortunately, the surge did not reach that level.
“It’s clear that social distancing had a big impact on decreasing the doubling rate of reported cases,” he says.
The hospital capacity tool was simultaneously released on the internet and accessed by hospitals for early planning needs throughout Washington as well as by researchers in Brazil and South Africa.
“The nice thing about this model is that it’s a simple and flexible tool—you don’t have to wait for someone else to run it for you,” Amram says. “And, it’s not COVID specific—it can be used for modeling any other disease and it’s still here in case a second wave of COVID occurs in the fall or winter.”
Washington hospitals and public health officials can also gain valuable information from a vulnerability index tool developed by fellow CHaSE Lab epidemiologist Pablo Monsivais, an associate professor in the Department of Nutrition and Exercise Physiology.
Monsivais says last March, he and Amram began analyzing community characteristics that could make people more vulnerable to the coronavirus.
The result was an interactive map of Washington neighborhoods color-coded to show where COVID-19 infections could lead to more severe outcomes and death. Monsivais says risk factors include high population density, an older demographic, and a greater prevalence of chronic conditions like heart disease, diabetes, pulmonary disease, or obesity.
Using census tract data, death records, and detailed geographic information, he calculated the disease burden for each community with hot spots in the Puget Sound area, for example, likely tied to high population density, while those in eastern Washington link to older populations with chronic diseases.
“This is really an infectious epidemic colliding with a chronic disease epidemic,” says Monsivais. “The biggest health problem in our society is not infectious disease but chronic disease—and those with pre-existing heart disease are among the most likely to suffer adverse consequences of COVID-19.”
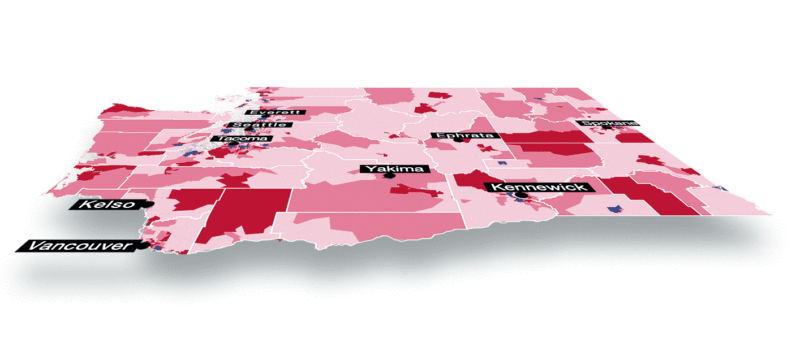 Example vulnerability index for COVID19 map (Courtesy CHaSE Lab)
Example vulnerability index for COVID19 map (Courtesy CHaSE Lab)



