Washington State University has embarked on one of its most ambitious expansions. The Elson S. Floyd College of Medicine is carving out its physician-training niche by emphasizing innovation, technology, and the importance of bringing high-quality care to some of the state’s most underserved regions.
The request came last spring.
Jim and Linda Bauer have opened their home to visiting symphony musicians, international artists, and others traveling to the Tri-Cities, and community leaders were turning to them again. This time, the Bauers were asked if they’d host a medical student for a weeklong stay at their Richland home.
“We were like, ‘Of course,’” recalls Linda Bauer, a retired U.S. Department of Energy employee. Her husband, also a retiree from the nearby Hanford Nuclear Reservation, adds, “We enjoy having visitors and hosting get-togethers.”
This, however, was different and the couple knew it.
The region has long identified physician recruitment as a top priority, and with Washington State University designating the Tri-Cities as one of four regional hubs for its new medical school, it would be a chance to make a lasting impression.
The Bauers were ready.
When student Kiah Jones arrived in September for a week of community immersion and instruction along with several of her classmates on the WSU Tri-Cities campus, a packed social calendar was waiting as well: visits with members of the local medical community, tours of the diverse Tri-Cities region, and even a Friday night concert inside a decommissioned nuclear reactor.
“We’re transplants from the Midwest and we love it here,” Linda Bauer says. “We know that if people take the time to learn about Eastern Washington, experience what it has to offer, they’ll love living here, too.”
Similar introductions were being made throughout the state as the inaugural class of 60 students from the Spokane-based Elson S. Floyd College of Medicine packed suitcases, grabbed their textbooks, and spent the third week of their first semester learning about the communities that desperately hope they’ll be back.
Washington State’s grand experiment in community-based medical education is underway.
FROM THE BEGINNING, WSU promised a different kind of medical school. A program committed to carving its own niche in physician training by emphasizing innovation, technology, leadership, and the critical importance of bringing high-quality care to underserved communities.
It had collaborated for years with the University of Washington’s medical school, but the two parted ways in 2014 over continuing differences in how best to address worsening physician shortages.
Clearing the way was former WSU President Elson S. Floyd’s successful push in 2015 to convince the Washington legislature to authorize and support a second public medical school for the state. Floyd, who had been battling colon cancer throughout the lobbying effort, died a few months later and other University leaders picked up where he left off, meeting tight deadlines to win national accreditation in 2016 and begin accepting student applications for the planned fall 2017 launch.
The commitment to primary care and underserved communities is what appealed to Jones, the medical student who spent a week with the Bauers in the Tri-Cities.
“I’d originally thought I wanted to do medical research,” she explains.
But during her junior year at Central Washington University, where she played intercollegiate volleyball when she wasn’t studying cellular and molecular biology, Jones became immersed in an intensive laboratory-based research project and discovered something important about herself: “I need to work directly with people.”
Her career goals shifted to clinical medicine, and having grown up in Port Angeles she understands what it’s like to live and work in small towns.
“My grandfather, actually, is who told me I should be looking at WSU,” Jones says.
Her undergraduate adviser and others, however, cautioned that the medical accreditation deadlines WSU faced were so tight that it was questionable whether the school would be ready to admit students for the 2017–18 academic year.
Nonetheless, Jones’ grandfather continued to provide regular updates on the school’s progress.
“He told me that everything I’ve been saying about why I want to go into medicine is what WSU is emphasizing,” she recalls.
When the Liaison Committee on Medical Education granted preliminary accreditation in October 2016, the traditional application period for U.S. medical schools already was underway. Jones’ grandfather called her immediately.
“I think the announcement had just been made,” she laughs. “I promised him I’d take a look, and when I got home I started reading everything I could. It was incredible; he was right.
“It was like someone had designed a medical school specifically for me.”
FOCUSING ON RURAL AND PRIMARY CARE was no accident.
The nation’s medical schools, physician residency programs, and others have struggled for years to boost the number of physicians practicing in rural and other underserved settings. Yet each new study shows fewer doctors setting up shop in America’s small towns.
A study commissioned by WSU in 2014 found the problem particularly acute in Washington, where the population continues to grow faster than the national average and too few in-state medical training opportunities were available for otherwise qualified students.
The problem is made worse by the disproportionate concentration of medical professionals in Seattle and King County, home to just 29 percent of the state’s total population but nearly half—49 percent—of its practicing physicians.
In the early 1900s, the legislature designated University of Washington as the sole public provider of physician training statewide. The UW medical school flourished and now is widely considered one of best in the world, featuring a faculty that includes three Nobel laureates.
But enrollment capacity had been largely limited even as the state’s population swelled. The 2014 study noted that increasing numbers of qualified students were having to leave Washington each year to enroll in out-of-state medical schools because there was no room for them here.
In Spokane, efforts to expand physician training as part of the collaboration between WSU and UW had mixed results, leading Floyd and others to begin pushing for greater control over medical education and curriculum. The two universities ended their partnership in late 2014 to pursue separate Spokane expansions.
“WSU has always had a significant health science focus so something like this wasn’t that big of a stretch,” says former WSU Spokane Chancellor Lisa Brown, a former state Senate majority leader who oversaw establishment of the new medical school in Spokane. “We train nurses and pharmacists and veterinarians and all kinds of other health professionals. We’re already doing amazing medical research here and on our other campuses. This is a logical next step.”
In fact, WSU earlier had moved its nursing and pharmacy schools to the Spokane campus along with other health science programs and much of the infrastructure already was in place to support a new medical school even before it received state approval. The effort also had the backing of the Spokane community, which had made increased medical education and research a top economic development priority.
The plan involved more than simply increasing educational capacity.
University leaders had been studying a new model that other states had pioneered over the past decade or so with what initial indications suggest could be promising results.
Community-based medical schools differ from the traditional model in that they rely on educational partnerships with existing hospitals and clinics rather than development of university-owned medical centers.
Instead of receiving their clinical training and experience in a central university hospital, for example, students spend their third and fourth years of medical school working alongside veteran physicians within communities where healthcare services are most needed.
The model was seen as a solid fit for WSU, a land-grant university with branch campuses and other facilities throughout the state that could help support the community-based approach.
In 2014, a group of WSU leaders toured Florida State University’s community-based medical school in Tallahassee and liked what they saw.
“The students were out in the communities, getting experience and developing relationships where their skills are most needed,” Brown explains.
The model had another advantage that Brown, a veteran of Olympia budget battles from her years in the legislature, recognized as well: “This was a way to operate a medical school without requiring a major capital investment in a university hospital.”
NEARLY 1,800 MILES AWAY, Dr. John Tomkowiak had heard about WSU’s interest in community-based medical education. Tomkowiak, dean of Chicago Medical School at the time, had built a reputation as an innovator and advocate for developing curriculum and training that keeps up with the rapid pace of change within the healthcare industry itself.
Before moving to Chicago, he held administrative and faculty roles at what was then a fledgling Florida State medical school and became a widely recognized proponent for community-based medical education.
Not surprisingly, Tomkowiak quickly emerged as a finalist in the nationwide search for a founding dean of WSU’s medical school. His hiring was approved by the Board of Regents in September 2015 and the task that awaited him was immense.
“I immediately saw it as this great opportunity,” says Tomkowiak. “It was this chance to start from the ground up. We’re able to ask ourselves, and our community partners, what does the doctor of the future look like, and then create a medical school that prepares them for that.”
At WSU, student innovation and entrepreneurship is being fostered.
Students will participate in problem-solving exercises known as hackathons where they’ll be presented with a current medical industry problem and given a fixed amount of time to brainstorm solutions. Ideas that might hold commercial potential will be nurtured along through a health technology incubator being developed on campus to help entrepreneurs.
“Literally, we are training the next generation of healthcare leaders and we want them to think big,” Tomkowiak says. “We want our students to not only learn about how to take care of patients but to focus on entire systems.”
Leadership is considered key.
WSU is among the first medical schools in the nation to require leadership training for graduation.
Doctors often are asked to take on leadership roles within hospitals, their own medical practices, and within their communities as well, Tomkowiak says, but typically have little or no preparation for that.
The curriculum also includes an emphasis on technology, including video consultations with patients in remote settings, and the use of composite data to identify health patterns and trends specific to a community that should be monitored or addressed.
“The more you practice, the better you get,” he says. “Our students will know how to use data to develop information that helps keep people well.”
EACH OF THE STUDENTS in the charter class hail from Washington.
In the rush to get the medical school ready for a fall 2017 launch, the University was so focused on serving regional needs it never developed an out-of-state tuition rate.
“Didn’t even think about it,” WSU President Kirk Schulz told students, their families, and others during a gathering in Spokane just before fall semester began. “We’re going to continue that commitment.”
Much like the school itself, the first class of students represents a departure.
More than half are female, all but two of the sixty grew up in medically underserved counties, 11 are first-generation college graduates, and a third are from low-income backgrounds, according to enrollment records. They range in age from 21 to 36 and bring a variety of undergraduate backgrounds.
Keely Coxon, for example, had her own public relations company before deciding to return to school in 2014 to finish needed prerequisites for medical school.
She grew up near Everett and had been interested in medicine when she enrolled at the University of Utah after graduating from high school in 2005 but eventually was drawn to writing and graduated with a degree in communications.
“When I was starting out, I looked at startups and nonprofits, I think because I liked giving people a voice,” says Coxon, a competitive runner and Alpine skier lured to Utah by the Wasatch Mountain Range. “But you end up taking on more projects on the Fortune 500 side.”
Then in 2011 her mother was diagnosed with a rare heart condition. The experience of researching the diagnosis and being there with her mom through genetic testing and treatment rekindled Coxon’s interest in medicine.
She later re-enrolled at Utah to complete the prerequisite coursework she’d need for medical school. Her microbiology professor, aware that she planned to take a year off between her postbaccalaureate studies and medical school, encouraged her to consider laboratory jobs because it would provide valuable exposure to the healthcare field and Coxon ended up at a pathology lab back in Everett. Her professor’s advice was solid. “The great thing about working in pathology is you get to see a lot about every field,” Coxon says.
Friends and family, meanwhile, had kept close watch on WSU’s progress and urged her to apply.
“I think my mom just wanted me back in Washington,” Coxon says with a laugh. “The day they got their accreditation, she called me.
“I’d been watching it too and there was something about the way they were doing their curriculum. I just had a good feeling about it.”
IN AUGUST, Elson S. Floyd’s wife, Carmento, traveled to Spokane to meet the inaugural class of medical students.
In the final months of her husband’s life she’d celebrated with him the legislative victory that enabled WSU to begin creating its own medical school, and reflected again on the accomplishment, this time alone, when it received national accreditation.
Each of the students in the charter class had been individually interviewed by WSU faculty and administrators, but she wanted to make sure they understood that her husband’s legacy is now in their hands.
“My husband…believed that if greatness can be accomplished it can be accomplished at Washington State University,” she said, tearfully. “Your journey…fulfills his dream.
“We expect greatness from you and you must expect greatness from yourselves.”
Nearby, student Sam Bloomsburg contemplated the final months of Elson S. Floyd’s life, what it must have been like to continue pushing for something so ambitious while battling a terminal condition and realized that Carmento had been as much a part of that journey as anyone.
“I was surprised by how much it affected me,” says Bloomsburg, who was raised in suburban Bellevue but got a hands-on introduction to rural healthcare this past summer shadowing a family physician in northern Idaho.
He approached Carmento Floyd during the Spokane event and hoped he could adequately convey his and his classmates’ gratitude.
“I went up to her and all I could think to say was, ‘Thank you for everything you and your husband did,’” Bloomsburg explains. “She was very gracious. I just thought it was important for her to know we recognize the opportunity we’ve been provided.”
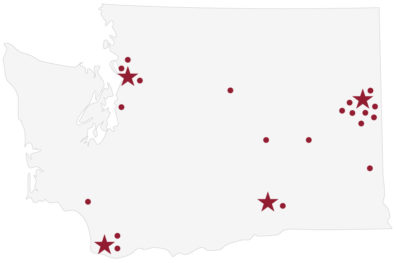
Distributed clinical campuses (Courtesy Elson S. Floyd College of Medicine)
Web extras
Medical leaders keep a community-based focus
Host families give a boost to WSU med students (The Spokesman-Review)