For the better part of four decades, Mark Wildung (’89 BS, ’92 MS) felt lousy.
He felt like he had a flu, but wrote it off, thinking everyone felt that way. He had a hollow leg, packing twice as much food as his friends on backpacking trips, but his body was withering away, his weight dropping to 138 pounds.
Finally, at a going-away party before a trip to Germany, a physician-assistant friend suggested he might have celiac disease, an autoimmune reaction to certain gluten proteins found in grains like wheat, barley, and rye. His symptoms got worse in Germany, a land of great bread and beer, and he confirmed he did indeed have the disease.
“When I was diagnosed, my ability to absorb nutrients had stopped,” says Wildung, 47. “I was eating, I don’t know, well over 5,000 calories a day and losing weight.”
Back in Pullman, where he is senior scientific assistant in the WSU Genomics Core Lab, he ended up deciphering genetic codes of wheat that the lab of Diter von Wettstein is investigating to develop a grain that celiac patients can safely eat. As it happens, the lab is making some of the greatest progress in the world on the problem.
About one in 100 Americans have celiac disease, with more diagnosed each year as awareness of the condition grows and the phrase “gluten free” permeates the food marketplace. In addition to weight loss, symptoms can include diarrhea, a distended abdomen, osteoporosis, and anemia. There’s no treatment other than a complete abstinence from gluten-containing grains.
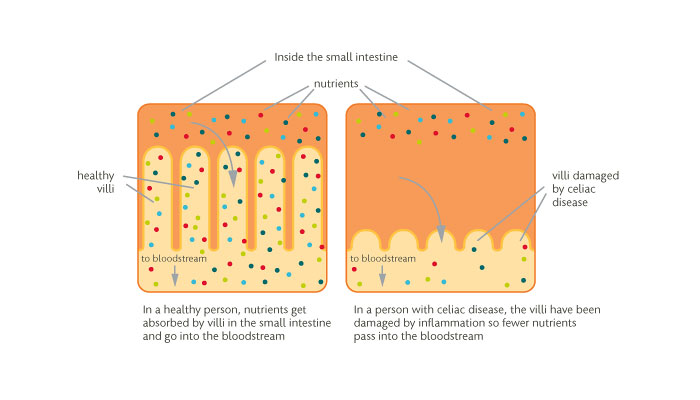
At the heart of the problem are certain proteins that aggravate microvilli, hair-like membranes through which the small intestine takes up nutrients. Through an autoimmune reaction, a celiac patient’s gut in effect erases the microvilli, creating what Wildung calls “smooth pipes.”
While gluten generally gets blamed for the problem, not all glutens are alike when it comes to celiac disease. Gluten comes in two basic forms, glutenins and gliadins. And it turns out that celiac patients generally don’t have a reaction to high molecular weight glutenins, which conveniently are enough to give wheat its baking properties. So in theory, one could have a non-toxic, nearly gliadin-free bread that bakes just fine.
Writing last fall in the Proceedings of the National Academy of Sciences, Sachin Rustgi, an assistant research professor, reported with von Wettstein and other colleagues that they could turn off a gene responsible for the creation of the toxic proteins but leave the high molecular weight glutenins.
“It’s like a process of production,” explains Nuan Wen, a doctoral candidate in molecular plant science and a co-author on the paper. Once the gene is turned off, she says, “it’s like the machine is locked.”
This method might knock out 75 percent of a grain’s toxic proteins, says Rustgi. It’s a step in the right direction, but it might not be enough.
“It may be useful material for some of the celiac patients because not all proteins are toxic to all patients,” he says. But it’s hard to say which patients will be good enough with just gliadin- or glutenin-free wheat.
So the researchers are also working on a way to have certain enzymes degrade the toxic proteins into smaller, non-toxic units. Stanford University researchers have developed similar enzymes that can be taken as a dietary supplement, but the WSU researchers are working to get a plant to synthesize the enzymes in the grain itself.
“You’re actually degrading everything into amino acids and leaving it non-toxic for humans” with celiac disease, says Rustgi.
By making the grain’s proteins more digestible, the work could make wheat more nutritious.
“It’s a fringe benefit,” says Rustgi. “Not only can wheat be less toxic for celiac patients, it can be more nutritious for everyone. Maybe eating one bread slice, you will get enough, when earlier you were eating two bread slices.”
A third approach would directly target the genes responsible for the toxic proteins by breeding a grain without them.
For his part, Wildung is most excited about what a bread tolerable to celiac patients means to von Wettstein, “a loves-science kind of guy,” and his team. And while Wildung would be able to eat bread again, other celiac sufferers would be able to eat it without enduring the travails of illness and a diagnosis.
On the web
WSU Department of Crop and Soil Sciences
Infographic of celiac disease intestine